Why Extreme Temperatures Are Becoming India’s Next Maternal Health Emergency
Author: Pallavi Sharma, Consultant, Tarutium Global Consulting
India is getting hotter. That is no longer debated. What remains dangerously under-recognised is who pays the highest biological price for this heat, and how early that cost is being paid.
In recent years, India has experienced some of its most intense and prolonged heatwaves on record. Summers now routinely push temperatures beyond human comfort and, increasingly, beyond human safety. In 2024 alone, temperatures crossed 50°C in parts of the country, with tens of thousands of suspected heatstroke cases reported. These numbers are often treated as environmental or disaster statistics. Rarely are they read as maternal health data.
In a warming India, pregnancy itself is becoming a high-risk condition, not because women’s bodies are failing, but because our health, labour, and climate systems have failed to recognise extreme heat as a maternal threat.
Heat Is Not Just Uncomfortable. It Is Physiologically Dangerous in Pregnancy.
Pregnancy fundamentally alters how the body responds to heat. Blood volume increases, the cardiovascular system works harder, and thermoregulation becomes less efficient. These changes, normal and necessary for foetal development, also make pregnant women less able to tolerate high ambient temperatures.
Growing global and Indian evidence now links exposure to extreme heat during pregnancy with:
- preterm birth
- stillbirth
- hypertensive disorders, including pre-eclampsia

- low birth weight and restricted foetal growth
The pathways are increasingly clear. Heat accelerates dehydration, thickens blood, and reduces placental perfusion. Cardiovascular strain rises as the body struggles to cool itself. Inflammatory and hormonal responses triggered by heat stress may precipitate preterm labour. With sustained exposure, foetal development itself is compromised.
These are not rare or theoretical risks. They are predictable outcomes of sustained heat exposure during pregnancy.
Yet in routine antenatal care across India, women are screened for blood pressure and haemoglobin, but not for heat exposure. Environmental stress remains invisible in maternal health protocols, even as temperatures climb year after year.
Today, heat exposure is not routinely captured in India’s maternal health data systems, including HMIS, antenatal registers, or high-risk pregnancy tracking systems. As a result, the contribution of extreme heat to adverse pregnancy outcomes remains largely invisible in official statistics. Until heat exposure is recognised as a reportable maternal risk, policy responses will continue to underestimate its impact.
Where Climate Meets Inequality: Who Bears the Heat Burden
Extreme heat does not affect all pregnant women equally. Its risks are socially patterned.

Nearly 90% of working women in India are employed in the informal sector – agriculture, construction, brick kilns, factories, street vending, and domestic work. For millions of pregnant women, work continues through pregnancy not by choice, but by necessity. Wages are earned daily. Food, rent, and survival depend on showing up. This work is overwhelmingly heat-exposed:
A BBC report captures this reality through the words of a pregnant agricultural worker in Tamil Nadu: “My hands burn in this heat.” The statement is simple, but it carries the weight of structural neglect. Heat here is not a passing discomfort; it is a daily, embodied stress etched into the body.
The same report documents the experience of another woman who experienced a stillbirth at six months of pregnancy after sustained work in extreme heat. Her story is not an anomaly. It is a warning.
Paid labour is only part of the exposure. Unpaid work – fetching water, cooking, caring for children, travelling to ration shops and health facilities – continues relentlessly. Overcrowded homes with heat-trapping roofs offer little relief. For many pregnant women, there is no cool space, no safe pause from heat, anywhere in the day.
Heat, in this context, is not just an environmental factor. It is a structural determinant of maternal risk.
Why Existing Systems Are Falling Short
India is not lacking in maternal health programmes or legal protections. The National Health Mission, Pradhan Mantri Surakshit Matritva Abhiyan, and the Maternity Benefit Act collectively represent decades of investment in maternal and child health.
These frameworks were not designed for a climate where extreme heat is no longer episodic – it is routine.
- Maternal health programmes rarely account for environmental exposure.
- Labour protections seldom recognise thermal stress as a workplace hazard for pregnant workers, particularly in informal employment.
- Heat Action Plans exist in many states but are largely disconnected from maternal health and labour systems.
As a result, heat falls between sectors. It sits in the environment or disaster domain, while quietly shaping pregnancy outcomes without accountability or ownership.
Beyond health outcomes, heat-related pregnancy complications also carry long-term economic consequences, through increased healthcare costs, productivity loss, and intergenerational impacts on child health and human capital.
From Coping to Protection: What Must Change Now
If India is serious about safeguarding maternal health in a warming world, incremental coping advice is no longer enough. What is required is systemic protection.
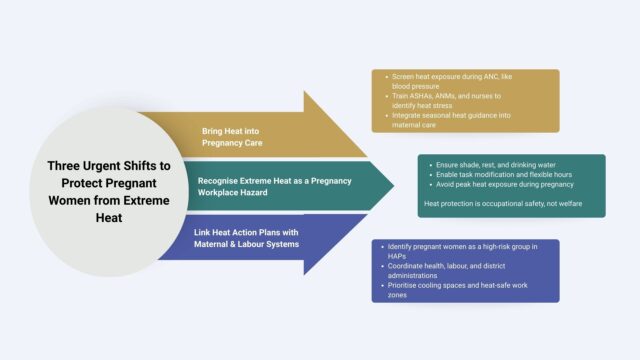
Three shifts are urgent and achievable:
- Bring heat into pregnancy care
In heat-prone districts, screening for heat exposure must become as routine in antenatal care as blood pressure measurement.
Frontline workers – ASHAs, ANMs, nurses should be equipped to recognise signs of heat stress in pregnancy and counsel women on risk reduction. Seasonal heat guidance must be integrated into maternal health communication and high-risk pregnancy monitoring.
- Recognise extreme heat as a pregnancy-related workplace hazard
Extreme heat must be formally acknowledged as a workplace risk for pregnant workers, including in informal settings.
This requires clear guidance on:
- access to shade, rest, and drinking water
- modified tasks and flexible hours
- avoidance of peak heat exposure during pregnancy
Protecting pregnant workers is necessary to ensure occupational safety.
- Link Heat Action Plans with maternal and labour systems
District and state Heat Action Plans must explicitly recognise pregnant women as a high-risk group.
Local coordination between health departments, labour offices, and district administrations is essential. Community cooling spaces and heat-safe work zones should be prioritised in areas with high concentrations of informal women workers. It requires existing systems to recognise a new reality.
Heat Is Already Shaping the Next Generation
When pregnancy unfolds under extreme heat, climate change is no longer abstract. It shapes blood pressure, birth timing, fetal growth, and survival. It shapes the health of the next generation before birth.
Protecting pregnant women from heat is not an “additional” concern. It is central to maternal health, to climate adaptation, and to what equity must mean in a warming India.
Addressing this crisis requires shared ownership, from health ministries and labour departments to urban planners and climate authorities, because heat does not respect sectoral boundaries, and neither do its impacts on pregnancy.
If we continue to ignore heat as a maternal health risk, we are not merely unprepared for climate change. We are complicit in allowing preventable harm to begin in the womb.
This is the moment to act. The temperature is rising. So are the stakes.


